|
A clinicopathological correlation (CPC) can be described as an objective summary and correlation of clinical findings with gross and microscopic findings and with the results of other studies performed at autopsy, to describe the death and elucidate the sequence of events leading to death33. A discussion or listing of the underlying cause or causes of death and the immediate cause should be included in the summary. This is additional to the stated cause of death in ONS format. Not all autopsy reports include such a commentary which, if present, is usually placed at the end of the report.
Sixty one percent (1,025/1,691) of the autopsy reports included a CPC, the majority of which were clearly expressed, consistent with the factual contents of the report and relevant to the circumstances of the death. This is similar to figures quoted in previous NCEPOD reports.
When the score given by advisors for the overall quality of the autopsy report was correlated with whether or not the report contained a CPC, it was found that those cases that contained
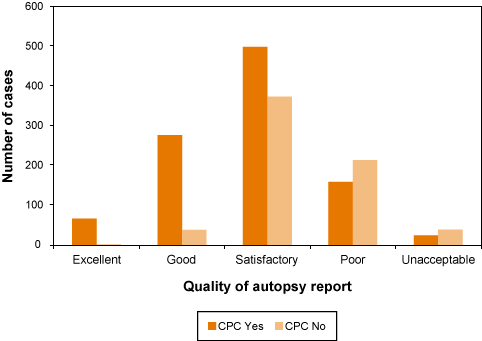
a CPC were associated with an overall better report score. In fact, all of the cases scored as 'excellent' contained a CPC (Figure 12).
Figure 12: Overall quality of the autopsy reports in cases that did or did not include a clinicopathological correlation
The inclusion or exclusion of a CPC, like the inclusion of a clinical history at the beginning of the autopsy report, is variable. As early as the 1995 NCEPOD report there was a recommendation stating:
"A concise, jargon-free explanation of the principle findings (clinicopathological correlation) should be a part of every post mortem."34
The same recommendation has been repeated in a number of NCEPOD reports since then, but the rate of inclusion of such a correlation has never exceeded 68%.
The Royal College of Pathologists also support the inclusion of a CPC, stating in their Guidelines that:
"It is probably the most important part of the autopsy report for the clinician and often the coroner"3.
The American College of Pathologists33 also support the inclusion of a CPC. Their guidelines state:
"Interpretation or explanation of autopsy findings may be crucial for educational and quality improvement purposes and to further explain the cause and manner of the patient's death. Anyone reading the autopsy report hopes to learn the cause and manner of the patient's death. It is our opinion that a clinicopathologic summary built around objective documentation is an appropriate and important endeavour for the pathologist."
One standard text4 on the coronial system also emphasises the importance of including
a summary and conclusion in an autopsy report:
"A brief well written summary is often of considerable use to the coroner. In many cases it is unnecessary to call the pathologist to give oral evidence at court [i.e. at inquest] and a straightforward summary can be read out as the evidence [under Coroners Rule 37]. On the other hand, a report without a summary - or a summary written in incomprehensible medical terminology - presents the court with a difficulty... It is preferable for the pathologist to phrase the summary in such a way that everyone in court, most particularly the relatives of the deceased, can understand the medical cause of death'.
Examples of good correlations have been provided in previous sections.
Providing a comprehensive and comprehensible CPC benefits all the interested parties.
The coroner can better understand a complex case, particularly important in perioperative deaths as has been indicated in all previous NCEPOD reports that included pathological assessment, and the relatives are more likely to come to terms with the death if they understand what happened. Finally, the pathologist is compelled to review all the circumstances of the case and attempt to account for all the features. If there are features which remain unresolved even after the autopsy and any further investigations, they can be honestly indicated.
There is a caveat which needs to be stated. Due to the way the autopsy reports and supporting documentation were collected, there was no way of knowing which cases would and did end up with an inquest (on a statistical basis, 10-12% would have eventuated in a public inquest). At inquest, the autopsy report (as seen in the study) forms the basis of the pathology evidence, but questions can be asked of it by the coroner and other interested parties; the findings can be challenged and the conclusions changed. It is possible that a proportion of the cases without CPC were those where the pathologist was aware at the time of writing the report that an inquest would be held, and thus withheld a correlation. However this cannot be the main explanation as 39% (666/1,691) of the cases studied did not have this component; and even in cases going to inquest, it is still a useful positive exercise for the pathologist to document the areas of clarity and (if appropriate) of difficulty in the clinicopathological description of the death. It is not being made as a specific recommendation, but it would be helpful for all readers of autopsy reports if it were clearly stated if the report is not the final word from the pathologist, because an inquest has yet to be held.
Recommendation
There should be a clinicopathological correlation in each report that reviews the case and robustness of the conclusions based on the available evidence.
|

