APPENDIX D. DEATHS REPORTED TO NCEPOD
INTRODUCTION (back to top)Prior to 1 April 2002, NCEPOD collected data on deaths occurring within 30 days of a surgical procedure performed by a surgeon or gynaecologist. These data acted as a sample pool from which to select study cases. However, since 1 April 2002, the remit of NCEPOD has been extended to include medical as well as surgical deaths, regardless of whether
a procedure was performed. So for the first time since the inception of NCEPOD, data were requested on ALL inpatient deaths regardless of length of stay in hospital. This dataset
then acted as a sample pool from which to identify the cases of GI therapeutic endoscopy relevant to this study. The extension to the dataset resulted in a greater than tenfold increase in the number of deaths reported to NCEPOD on an annual basis and the sample endoscopy cases selected for this study represented only a small proportion of the data.
DATA COLLECTION (back to top)
The data presented in this chapter relates to all inpatient deaths occurring between 1 April 2002 and 31 March 2003. Data were reported from all acute NHS Trusts in England, Wales and Northern Ireland and Primary Care Trusts where appropriate. Data were also reported from Guernsey, the Isle of Man, the independent sector and the Defence Secondary Care Agency.
In each hospital a nominated member of staff acts as a local link between the hospital
and NCEPOD and is known as the NCEPOD local reporter. A member of the clinical governance, audit or information department most commonly fills the role as the data collection requirements of NCEPOD have evolved and the use of electronic data increased. Data on inpatient deaths was, in the majority, submitted on a password-protected spreadsheet, for which a template was provided. Whilst most hospitals were able to meet this request, in fact some found it easier than the previous data selection of 30 day deaths as no filtering was required, a small proportion of hospitals were unable to generate the information from their patient administration system (PAS). In such cases, a paper form
was completed for each death. As full electronic submission was a new process for NCEPOD some initial difficulties were to be expected. However, even after one year it was extraordinary that some hospitals were not able to provide basic information on patients
that had died in hospital either electronically or manually.
DATA ANALYSIS (back to top)
Exclusions
Unlike many previous NCEPOD reports, the criteria by which cases were excluded were minimal. Previously cases would have been excluded if the procedure was minor such as the insertion of an intravenous infusion or if a physician performed it. For the first time no such exclusions were made. However, only data returned before the deadline of 31 July 2003 were included.
Cleaning
Once data collection had closed, all data in the database were cleaned to ensure that the data in each field was of the same format and that date fields such as date of birth, date of admission and date of death were all in the correct order, e.g. date of procedure was after date of birth and before date of death, and procedure codes were held in the same way as the Hospital Episode Statistics (HES) data, to make comparisons easier. All duplicate records were removed.
OVERVIEW OF DATA RECEIVED (back to top)

Figure 22. Numbers of records received (inpatient deaths 2002/03)
This year saw a dramatic increase in the percentage of duplicate records submitted; 13% compared with approximately 1% last year (Figure 22). The main reason for this, which had not been predicted, was the ability to provide cumulative submissions with updated records during the year. As the PAS records became more complete, data were re-submitted to replace the record held. Duplicate records were accepted initially to ensure a more accurate dataset, only being deleted once the dataset was complete. The percentage of data returned after the deadline was very similar to last year: 0.5% compared with 0.4%.
Regional spread
Since the introduction of Strategic Health Authorities (StHA) the previous regional boundaries used by NCEPOD no longer apply. NCEPOD’s current database does not facilitate the display of deaths by StHA therefore Table 83 shows the number of deaths reported to NCEPOD by country or sector.
| Table 83. Number (%) of inpatient deaths by region | ||||||
| Region |
|
|
||||
England |
|
|
||||
Wales |
|
|
||||
| Northern Ireland |
|
|
||||
| Guernsey |
|
|
||||
| Jersey | No cases reported |
|
||||
| Isle of Man |
|
|
||||
| Defence Secondary Care Agency |
|
|
||||
Independent |
|
|
||||
Interestingly, it can be seen from Table 83 that despite the enormous increase in the total number of deaths recorded by NCEPOD, the percentage spread has changed very little, indicating a consistent return of data from hospitals.
Completeness of data
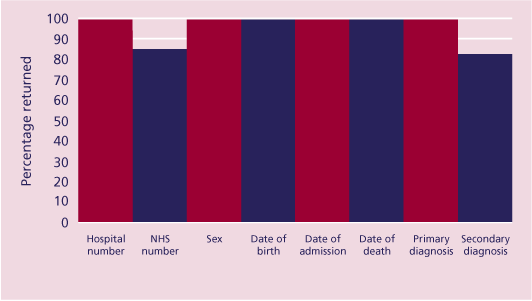
Figure 23. Completeness of data returned
The dataset was reviewed to determine how well fields were completed and the results
are displayed in Figure 23. Dates of birth and dates of death were obtained for all patients, as these were required fields. The hospital casenote number was absent in less than 1% (105/243,318) of records compared with the NHS number that was absent in 15% (36,573/243,318), although these include the majority of cases from the independent sector who do not use an NHS number routinely. Of the diagnosis fields, primary diagnosis was absent in less than 1% (199/243,318) of the cases compared with first subsidiary (secondary) diagnosis, which was absent 18% (43,377/243,318) of the time. The sex of
the patient could not be supplied in 8 (<1%) of the cases and the date of admission in
47 (<1%).
Age and sex
As the new remit included all deaths it was anticipated that a slight reduction in the mean age of patients would have been seen this year. However, despite the dataset being more than ten times larger, with a median (range) age of 80 (<1 to 109) years, the age distribution are comparable with those reported in previous NCEPOD reports (Figure 24).
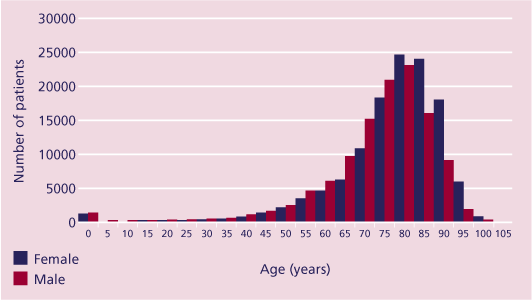
Figure 24. Distribution of age and sex (Inpatient deaths 2002/03)
Duration between admission and death
It can be seen from Figure 25 that more patients died during the first three days following admission than on any subsequent three-day period. Whilst that has been seen in previous NCEPOD reports following surgery, it is interesting to note that these data were similar regardless of whether a procedure was performed or not. It is likely therefore that this simply reflects the fact that many patients admitted to hospital, especially for no procedure,
are extremely ill.
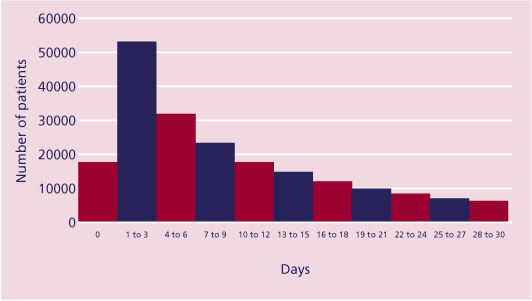
Figure 25. The duration between admission to hospital and death for all patients
Final primary diagnosis
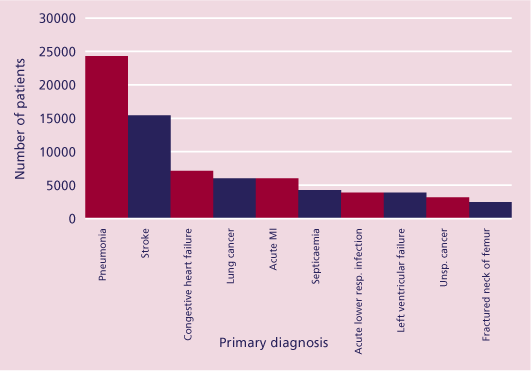
Figure 26. Ten most common final primary diagnoses
Figure 26 displays the most common primary diagnoses for inpatient deaths.
Procedures performed
For the dataset, we requested that the last six procedures prior to death be recorded. Of the 243,318 cases, 69,536 (29%) patients had at least one procedure performed. However, where data on procedures were not supplied it is not possible to state for certain that a procedure was not performed, simply that the data were not available.
COMPARISON OF DEATH DATA FROM NCEPOD AND HOSPITAL EPISODE STATISTICS
(back to top)
NCEPOD has previously been involved with comparative studies between the data submitted to NCEPOD and the data submitted to HES. These studies have shown inconsistent differences between the two datasets in reference to the number of deaths reported to each from the same Trusts. However, such comparisons have always been performed on specifically filtered data e.g. deaths within 30 days of a surgical procedure and any difference in definitions between the two datasets would automatically introduce errors. Therefore, as NCEPOD had data on all inpatient deaths for the 2002-03 data year, it was
felt to be a more robust dataset with which to compare the HES dataset of the same year. However, instead of comparing the total number of deaths reported to each dataset by
the same Trust, both datasets were sampled for cases of GI therapeutic endoscopy to determine whether by sampling directly from HES, the same sample group, as used in this report, would have been identified.
The HES dataset for all inpatient deaths in England NHS Trusts during 1 April 2002 to 31 March 2003 was obtained by NCEPOD following approval by the Department of Health’s Security and Confidentiality Advisory Group.
To ensure an accurate comparison only acute English NHS Trusts were selected from the NCEPOD and the HES datasets. This gave a total of 213,855 records from NCEPOD and
a total of 262,293 records from HES.
Both datasets were then sampled for the last therapeutic gastrointestinal endoscopy performed within 30 days of death, using the OPCS codes defined in the chapter outlining the study method.
Matching of the two sets of sample cases was then performed over a number of stages, described below. Whilst the ideal match would be based on a number of fields, the more fields added to match on, the more likely there would have not been a match due to slight differences in the data available and missing data. The method adopted was to match initially on only NHS number and casenote number and then to manually compare the
data to confirm the matched status by looking at the remaining fields.
| Stage 1 | Cases were matched if both the NHS number and the casenote numbers were identical. |
| Stage 2 | Cases were matched on NHS number alone. These were then checked manually to ensure the data in the other fields confirmed the match. |
| Stage 3 | The remaining unmatched samples from each dataset were compared with all the non-sample cases in the opposing dataset to determine if a match was not being found because it had not been identified as a sample case but was recorded as a death. |
| Stage 4 | All remaining samples that had not been matched to a sample case or to a death record were reviewed individually. Matching was attempted using date of birth, date of death and date of admission and comparing all fields in any matches to identify simple reasons why the cases had not matched, e.g. NHS number not available, casenote number was different, unavailable or had an additional letter in one dataset and the date of admission was different by one day. In such a case, the source hospital was checked to ensure that they matched and all fields were compared. If the records matched on hospital plus three other dates from birth, admission, death and procedure they were granted as matching. Figure 27 provides an overview of the results. |
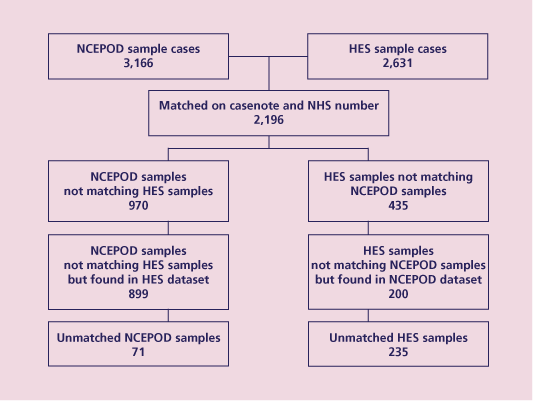
Figure 27. Overview of the samples obtained from comparing the NCEPOD and HES datasets
Of the 2,196 samples that matched, only 30 did not have the same type of endoscopy for the final endoscopic procedure e.g. one was upper GI and one was lower GI. Only 61 did
not have identical codes but were the same type of procedure e.g. PEG instead of upper GI, which was a common difference in coding.
Whilst an acceptable level of matching was found, the most common reasons for cases not matching were due to simple, yet important differences in the datasets. Often casenote numbers/NHS numbers were supplied in one dataset and not the other. More worryingly was that when the NHS number was not supplied, matching often failed because the casenote number was completely different, even though the cases were from the same hospital and were identical in every other way.
The most important points of concern to highlight from this analysis are that firstly, in 899 of the 970 unmatched NCEPOD samples the cases had been reported to HES but endoscopy procedure codes had not been provided. This may indicate that hospitals had been more diligent in ensuring that endoscopic cases were reported to NCEPOD; to check this, the analysis will need to be repeated using an unrelated sample group. However, it may also indicate that the HES data were cleaner. The data in HES are updated regularly throughout the year, which may mean that incorrect procedure codes had been removed. Secondly,
in 235 of 435 cases reported to HES, the death was not reported to NCEPOD at all. These cases will need to be analysed in more detail to identify why this discrepancy occurred and relay this information back to Trusts so that we can help ensure the robustness of future datasets.
It can be seen from these data that neither reporting system is perfect. However, more deaths were reported to HES than to NCEPOD and only 71 records in the NCEPOD dataset could not be found in the HES data, which is an encouraging finding that will hopefully be consistent when the analysis is repeated with a different sample group.
If NCEPOD had used the HES dataset as the sample pool then a significant sample would have been identified and could have been used for the study. The major concern is that of obtaining the data from HES. The data used in this exercise were not available until eight months after the end of the 2002-03 financial year. It would have been hard to expect a clinician to complete a questionnaire on a patient that they may have seen up to 20 months previously. However, with the advent of the new National Programme for Information Technology (NPfIT) system for hospitals it is hoped that in time data transfer will become quicker and more easily available and identification of problems in the datasets now can only work to aid that process.
FUTURE COLLECTION OF DATA ON ALL INPATIENT DEATHS
(back to top)
All data held by NCEPOD is done so with a firm respect and compliance with confidentiality laws, even though regulations such as the Data Protection Act (DPA) 19981 do not apply to data from deceased patients, NCEPOD applies the same policy to all patient data held. As the third principle of the DPA 1998 states that ‘data collected should be relevant to the purpose for which it is being collected and the quantity collected should be appropriate’ it has been decided that collection of data on all inpatient deaths should cease. NCEPOD will utilise alternative sampling methods for future studies. One method, and the initial approach, will be to request that hospitals sample directly from their patient administration system (PAS) and identify information relevant only to a particular study. A second option will be for NCEPOD to continue to work with the Department of Health’s Hospital Episode Statistics (HES) to identify what and why discrepancies between the two datasets occur so that in future NCEPOD may sample directly from HES. Due to the changing nature of NCEPOD studies it is no longer appropriate to routinely collect data on deaths occurring in hospitals and therefore on 1 April 2004 NCEPOD ceased collection of this dataset.
1 Data Protection Act 1998 – Principles. Information Commissioner’s Office, 1998. http://www.hmso.gov.uk/acts/acts1998/80029--l.htm#sch1ptI
| (back to top) |